|
Home • Research • Publication • Glossary • Contacts ______________________________________________
|
|
Computerized
Training Tools for Cryosurgery Despite the
continuous development of devices and techniques for minimally invasive
cryosurgery, modern cryosurgery frequently falls short of maximizing
cryodestruction to the target region, while minimizing cryoinjury to the
surrounding healthy tissues. Here, one of the most significant
difficulties—and probably the less intuitive obstacle to
overcome—is the design and generation of a frozen region to adequately
correlate with the shape of the target region and established criteria for
cryosurgery success. This line of research focuses on medical training and
education associated with planning and creation of the optimal 3D thermal
field for cryosurgery, for the benefit of the surgeon, the medical
researcher, and the clinical instrumentation developer. A computerized
training tool prototype is being developed, with the objectives being to
shorten the clinician’s learning curve, reduce practice time, enable
case studies on “what-if” scenarios, and enable revaluation of
past clinical procedures via a cryosurgery database. While the training tool
is designed for general purposes, due to its high clinical relevancy, a
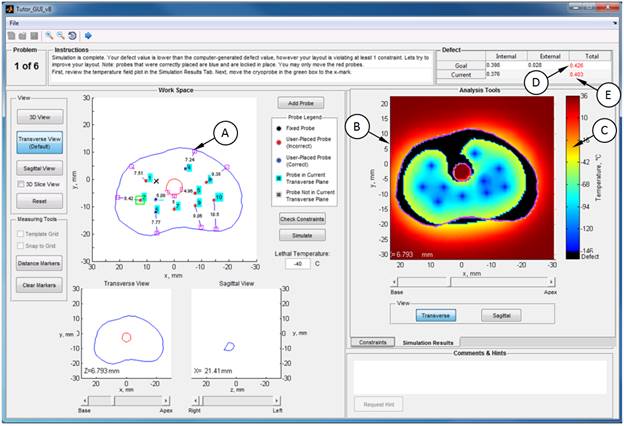
particular attention is paid to prostate cryosurgery. Below is a
representative screenshot from a recently developed intelligent tutoring
system (ITS) [PubMed]:
Selected
publications on computerized training tools for cryosurgery: •
Rabin, Y.,
Joshi, P., Sehrawat, A., Keelan, R., Shimada, K., Wilfong, D.M., McCormick
J.T. (2017): Evaluation of a Computerized Tutor Prototype for Prostate
Cryotherapy. Energy-based Treatment of Tissue and Assessment IX, SPIE –
BiOS 2017, San Francisco, CA, USA (January
28-Februrary 2) PubMed,
HHS Public Access, SPIE
Digital Library •
Sehrawat,
A., Keelan, R., Shimada, K., Wilfong, D.M., McCormick, J.T., Rabin, Y.
(2016): Simulation-based cryosurgery training: variable insertion-depth
planning in prostate cryosurgery, Technology in Cancer Research and
Treatment, 15(6):805-814 PubMed, HHS Public
Access, Sage •
Sehrawat,
A., Keelan, R., Shimada, K., Wilfong, D.M., McCormick, J.T., Rabin, Y.
(2016): Simulation-based cryosurgery intelligent tutoring system (ITS)
prototype, Technology in Cancer Research and Treatment, 15(2):396-407 PubMed, HHS Public
Access, Sage •
Keelan, R.,
Zhang, H., Shimada, K., Rabin, Y. (2016): GPU-based bioheat simulation to
facilitate rapid decision making associated with cryosurgery training,
Technology in Cancer Research and Treatment 15(2): 377-386 PubMed, HHS Public
Access, Sage •
Keelan, R.,
Shimada, K., Rabin, Y. (2015): GPU-based simulation of ultrasound imaging
artifacts for cryosurgery training, Technology in Cancer Research and
Treatment, 16(1):5–14 PubMed, HHS Public
Access, Sage •
Furuhata,
T., Song, I., Rabin, Y., Shimada, K. (2014): Interactive prostate shape
reconstruction from 3D TRUS images, Journal of Computational Design and
Engineering, 1(4):272-288 ScienceDirect,
BTTL
Depository •
Keelan, R.,
Yamakawa, S., Shimada, K., Rabin, Y. (2013):
Computerized Training of cryosurgery – a system approach, CryoLetters
34(4):324-337 PubMed,
HHS Public
Access •
Sehrawat,
A., Shimada, K., Rabin, Y. (2012): Generating
prostate models by means of geometric deformation for the application of
computerized training of cryosurgery. International Journal of Computer
Assisted Radiology and Surgery, 8(2): 301-312 PubMed, HHS Public
Access, Springer
Link •
Keelan, R.,
Shimada, K., Rabin, Y. (2011): Developing a
framework for computerized training of cryosurgery based on finite elements
analysis. ASME 2011 Summer Bioengineering Conference - SBC 2011, Farmington,
PA, USA (June 22-25) ASME
Digital Collection •
Sehrawat,
A., Shimada, K., Rabin, Y. (2011): Geometric deformation of three-dimensional
prostate model with applications to computerized training of cryosurgery.
ASME 2011 Summer Bioengineering Conference - SBC 2011, Farmington, PA, USA
(June 22-25) ASME
Digital Collection This
research has been supported, in part, by the National Cancer Institute, NIH
Grant # 1R01CA134261 |
|
______________________________________________ |